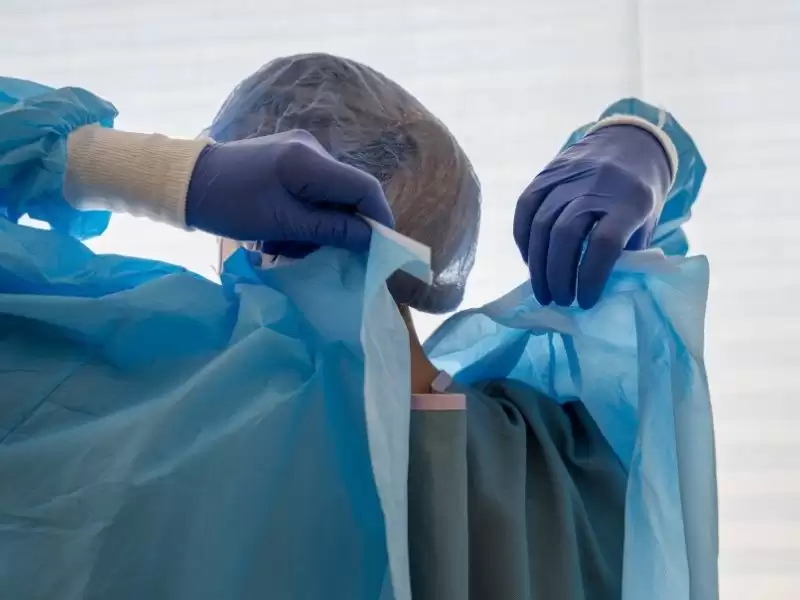
Microsurgical Cervical Disc Herniation Surgery
Cervical disc herniation surgery performed with microsurgery is recommended for patients who do not respond to medication or physical therapy and who have marked spinal cord and nerve root compression causing loss of strength in the arms.

In cervical disc herniation surgeries performed under general anesthesia, the right front side of the neck is usually used. A horizontal skin incision of approximately 3–4 cm is made. The surgeon proceeds between the neck muscles until the carotid artery is seen. In order to reach the spine, special instruments are used to move the carotid artery outward and the esophagus and trachea inward, allowing access to the front part of the cervical spine.
In order to identify the space between the vertebrae where the surgery will be performed, a marked X-ray is taken during the operation and the herniated area is determined. After this stage of the surgery, microdiscectomy is performed using a microscope to remove the herniated disc fragments compressing the nerves and spinal cord.


In cervical disc herniation surgeries, unlike lumbar disc surgery, the disc tissue between the two bones is completely removed. Therefore, prostheses or bone grafts are placed in place of the disc tissue in order to stabilize the two adjacent vertebrae. Afterwards, the surgical level is checked one final time with an X-ray, and after bleeding control, the incision site is closed in a way that does not require stitch removal, and the operation is completed.
The patient is helped to stand up in the 2nd hour after surgery with the aid of a neck brace to be used for two weeks, and is discharged one day later.